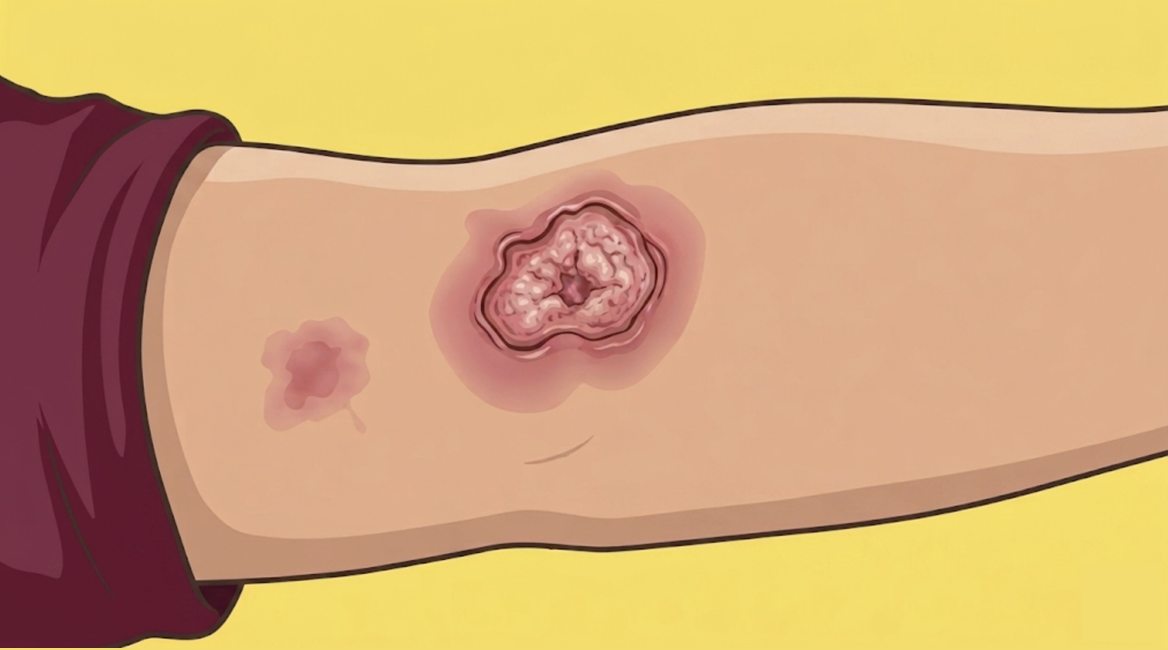
Cutaneous squamous cell carcinoma is the second most common skin cancer and develops due to mutations resulting in keratinocyte proliferation and expansion. In 1804, Rene Laennec described forms of skin cancer but it wasn’t until 1912 that the formal classification of squamous cell carcinoma in situ was used by John Templeton Bowen.
Etiology
- UV radiation (most common): cumulative long-term exposure, sunburns
- p53 mutation (most common genetic abnormality)
- Risk factors: UV exposure, increasing age, fair skin, immunosuppression, human papillomavirus (HPV) infection, solid organ transplantation, exposure to chemical carcinogens (e.g., arsenic, pesticides, asphalt, tar, ionizing radiation, tobacco use, HIV infection, etc.)
Epidemiology
- Average age: mid-60s
- Male predominance (3:1)
Pathogenesis
- UV radiation causes mutations and cellular changes leading to increased keratinocyte dysplasia
- p53 mutation allows keratinocytes to resist apoptosis and allow for expansion at expense of normal adjacent keratinocytes
- Histology → hyperkeratosis
- SCC in situ: full-thickness nuclear pleiomorphism
- SCC: invasion through basement membrane into dermis
Presentation
- Arises on sun-damaged skin in fair-skinned individuals → face, neck, bald scalp, extensor forearms, dorsal hands, shins
- Arises on chronic non-healing ulcers and scars in individuals with darker skin
- Erythematous or skin-colored, scaly patch, scaly papule (<1 cm), plaque (≥1 cm), or exophytic papillomatous nodule; associated crust, erosion, or ulceration may be present
- May be slow growing and nontender or rapidly enlarging and painful
- Inspect for satellite lesions and palpate regional lymph nodes
Diagnosis
- Skin biopsy
- Gold standard for diagnosis
- Approach
- Patch/thin plaque lesion → shave biopsy
- Papulonodular lesion → punch biopsy
- Histology
- cSCC in situ
- High-grade atypia of keratinocytes
- Lack of maturation at all levels of epidermis
- No invasive of atypical keratinocytes into underlying dermis
- Invasive cSCC: downward proliferation of atypical keratinocytes invading dermis
- cSCC in situ
Staging
- American Joint Committee on Cancer (AJCC-8)
- Applies only to cSCC on head/neck skin, vermillion lip
- Based on local tumor burden (T), nodal status (N), and metastatic disease (M)
- Tumor diameter >2 cm upstages tumor from T1 to T2
- High-risk features upstaging tumor to T3
- Tumor diameter >4 cm
- Minor bone erosion
- Invasion of nerves ≥0.1 mm in caliber or located in subcutis
- Deep tumor invasion (>6 mm or beyond subcutis)
- T4: involves major bone or skull bone invasion
- Bregham and Women’s Hospital
- T stage classified based on number of high risk features
- T1: 0 high risk features
- T2a: 1 high risk feature
- T2b: 2-3 high risk features
- T3: all 4 high risk features or bone invasion
- High-risk features in T classification
- Tumor diameter ≥2 cm
- Tumor invasion beyond subcutis
- PNI of nerves ≥0.1 mm in caliber and poor differentiation
- Doesn’t offer N or M staging criteria
- More accurately stratifies T categories based on outcomes
- T stage classified based on number of high risk features
Treatment
- Local tumor destruction → can be used for low-risk cSCC
- Low-risk cSCC definition
- <1 cm in diameter
- Superficially invasive to papillary dermis
- Located on trunk or proximal extremities
- Curettage and electrodessication (C&E)
- Requires 2-3 cycles
- Creates partial-thickness dermal wound that heals by secondary intention
- Does not allow for additional pathology as it is destructive
- Low-risk cSCC definition
- Excision
- Indications
- cSCC tumors without high-risk features
- cSCC in low-risk anatomical sites → trunk, extremities (excluding pretibial)
- <2 cm in diameter
- Margins
- Recommendation varies as there is no high-quality data to support
- Generally, recommend margin 0.4-0.6 cm
- Greater margin (~1.0 cm) is recommended for
- Tumors ≥2 cm
- Higher grade
- >1 cm located on scalp, ears, eyelids, nose, lips
- Indications
- Margin-controlled surgery
- Recommended for cSCC ≥6 mm depth or greater
- Await tissue rearrangement until negative margins are confirmed
- Total margin-controlled excision (TMCE)/Mohs micrographic surgery (MMS)
- Indications
- High-risk cSCC
- Incompletely excited tumors requiring re-excision
- Narrow histologic margins
- Tumors with high-risk features
- Treating recurrence would compromise cosmesis or function
- Reconstruction is usually done on the same day after the tumor is completely excised
- Note: radiation therapy may be used for incomplete margin control if additional surgery isn’t possible
- Indications
- Advanced disease
- Suspected nodal metastases
- CT with IV contrast C/A/P
- PET may be used when significant scarring/fibrosis
- FNA or core-needly biopsy
- Lymph nodes
- Regional lymphadenectomy → remove clinically apparent disease and remaining lymph nodes in the basin
- Nodal metastasis of head/neck, bulky lymphadenopathy (LN >3 cm), or multiple positive ipsilateral nodes → comprehensive ipsilateral neck dissection
- Radiation therapy (RT)
- Important for nodal metastasis → often use as adjunct following lymph node dissection
- Adjuvant RT recommended in patients with multiple positive lymph nodes or presence of extracapsular extension
- Systemic therapy
- Suspected nodal metastases
Relevant Information
- Second most common skin cancer (20-50%)
- Tumor diameter >2 cm doubles risk of tumor recurrence and triples rate of metastasis compared to tumors <2 cm in diameter
- Tumor depth is risk factor most highly associated with recurrence and metastasis
- Verrucous carcinoma
- A well-differentiated cSCC commonly associated with HPV infection
- Presents in older adults as large, exophytic verrucous plaque or nodule that grows gradually and pushes against and destroys underlying fascia and bone
- Three subtypes
- Epithelioma cuniculatum on plantar foot
- Giant condyloma acuminatum of genitalia or Buschke-Löwenstein tumor
- Oral florid papillomatosis of oral mucosa
- Histology: minimal cytologic atypia, tumor displays a pushing rather than infiltrate border
- Marjolin ulcer: from chronic healing wounds/burns
- Bowen’s disease
- Cutaneous SCC in situ
- More common on trunk, lower extremities, or genitalia
- Perianal lesions are associated with HPV
- Postoperative surveillance for local SCC
- Monitor every 3-12 months during first 2 years
- No new lesion → monitor every 6 months for the next 3 years
- Follow this by annual exam for life
Differential Diagnoses
- Seborrheic keratoses
- Benign adnexal tumors
- Prurigo nodularis
- Basal cell carcinoma
- Amelanotic melanoma
- Merkel cell carcinoma
- Lichen sclerosus
- Hypertrophic lichen planus
Resources
- Guidelines of Care for the Management of Cutaneous Squamous Cell Carcinoma (Journal of the American Academy of Dermatology, 2018)
- Squamous-Cell Carcinoma of the Skin (The New England Journal of Medicine, 2023)
- Squamous Cell Carcinoma Overview (The Skin Cancer Foundation)
- Basal and Squamous Cell Skin Cancer Stages and Risk Groups (American Cancer Society)
- AJCC Cancer Staging