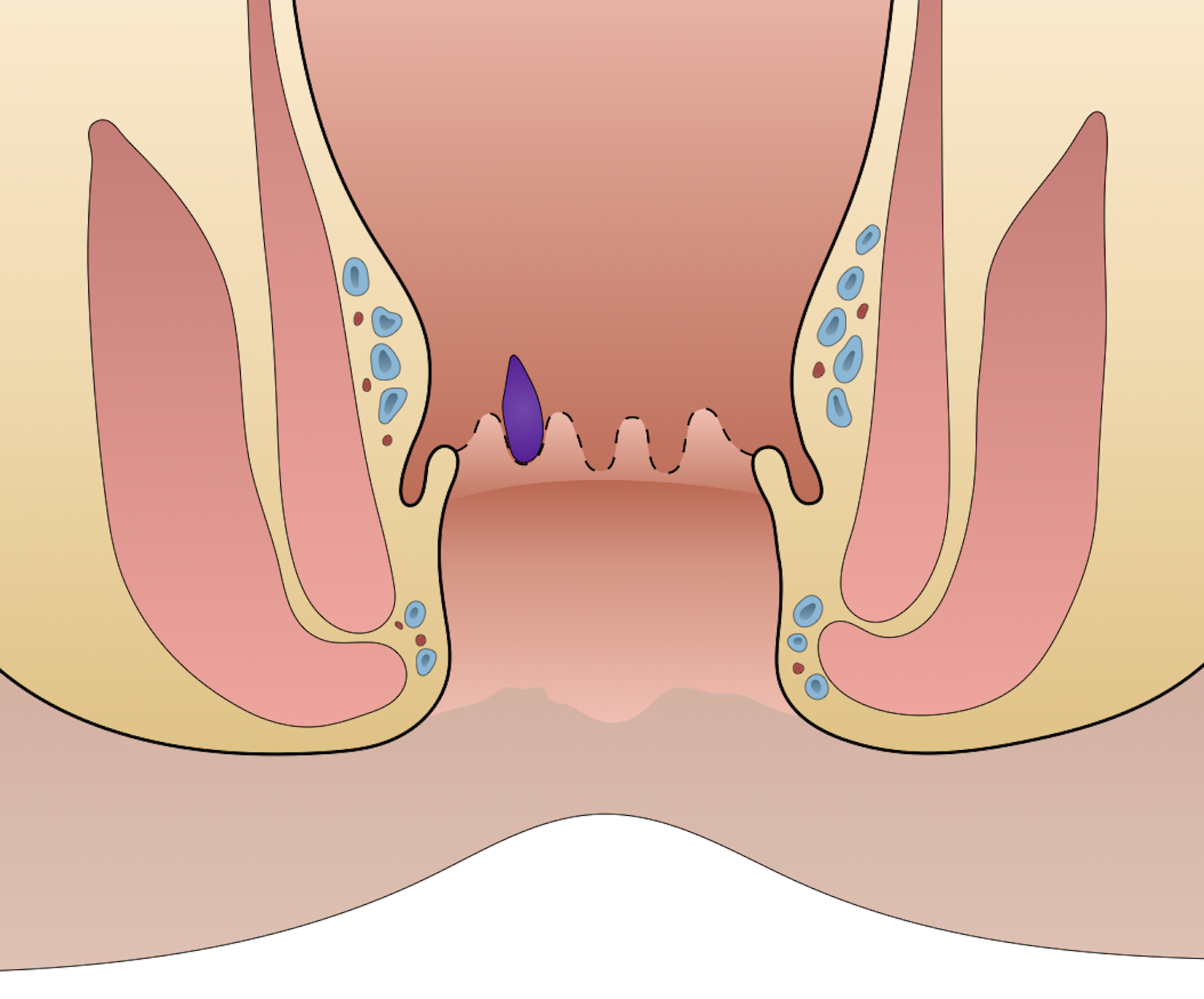
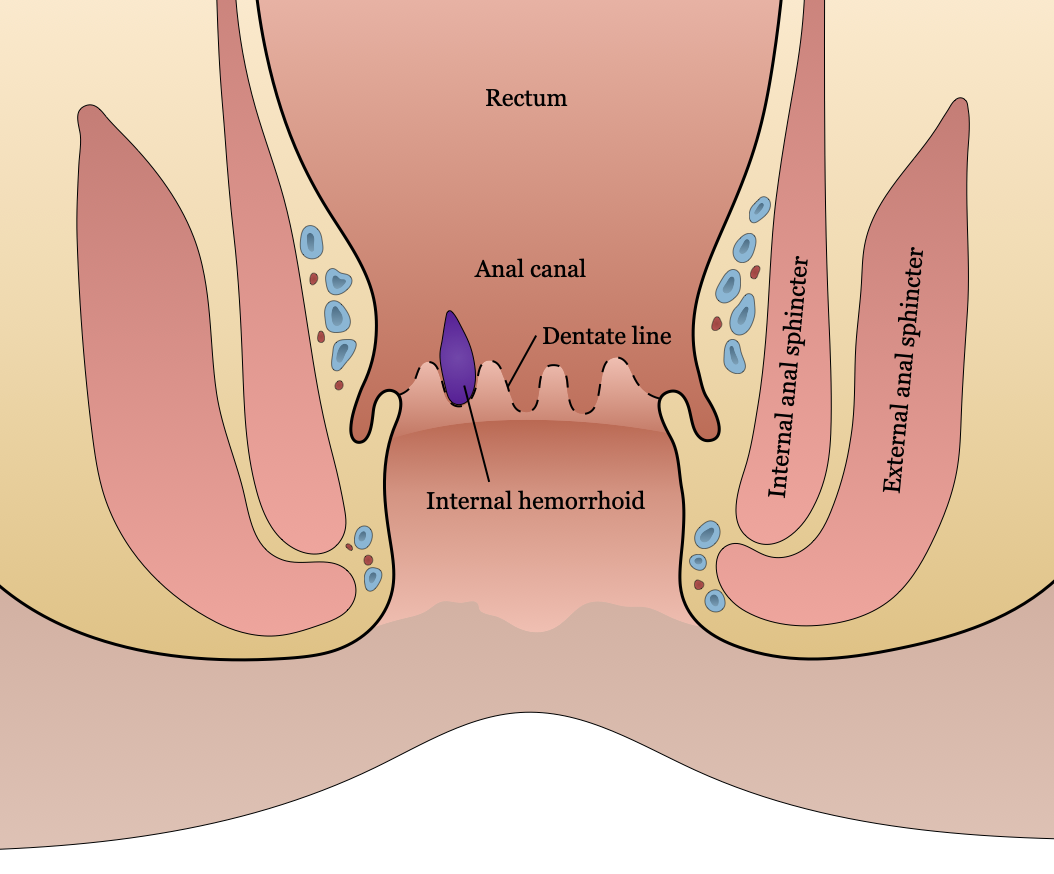
Internal hemorrhoids occur proximal to the dentate line. The treatment of hemorrhoids in the past has included suppositories, cautery, and excision. Walter Whitehead introduced a radical procedure in 1882 in which most of the area involved with the hemorrhoid was excised. Since 1882, additional approaches have come about. Notably, from Edward Campbell Milligan, James Morgan, and James A. Ferguson, among others.
Etiology
- Enlargement/protrusion of the anal hemorrhoidal cushions
- Risk factors: constipation, prolonged straining
Epidemiology
- Usually second or third decade
Pathogenesis
- Increased intraanal pressure leads to abnormal dilatation and engorgement of vascular channels
- Changes in the connective tissue within the anal cushions occurs as a result
- These changes cause an inflammatory reaction and vascular hyperplasia, which can be evident in hemorrhoids
- When the tissue that usually supports hemorrhoids fails, the anal cushion is displaced sitally and undergoes venous distention, erosion, bleeding, thrombosis, and/or tissue prolapse
History
- Painless bleeding with bowel movements
- ± Tissue protrusion
Physical Exam
- Visual inspection of anus
- Digital rectal exam
- Anoscopy
Treatment
- Begin with medical management
- Increased fluid intake (64 oz/day)
- Fiber supplementation: to increase bulk and caliber of stool
- Counsel on defecation habits (e.g., avoid straining, limit time on toilet)
- Sitz baths
- Witch hazel topical pads
- Continue with medical management for 6 – 8 weeks before considering more aggressive treatments
- Rubber band ligation
- Can be used for most patients with grade I and II internal hemorrhoids (and some patients with grade III)
- Office procedure
- Hemorrhoidectomy
- Closed (Ferguson) hemorrhoidectomy
- Open (Milligan-Morgan) hemorrhoidectomy: leaves mucosa open
Relevant Information
- History should be taken to include issues of perineal hygiene, fiber intake, bowel habits, including frequency, consistency, change in stool caliber, difficulty with evacuation, fecal incontinence

Differential Diagnoses
- Hemorrhoids, external
- Perianal abscess
- Fistulas
- Anal cancer
- Colon cancer
- Anal fissure
Resources
- American Society of Colon and Rectal Surgeons. “Clinical Practice Guidelines for the Management of Hemorrhoids,” (2024)