Ostomies are made when a portion of the GI tract is brought out through the abdominal wall, opened, and matured by suturing the wall of the bowel to the abdominal wall skin.
Ostomy Types
- Loop ostomy: loop of intestine is brought through abdominal wall, transverse incision made to open the bowel and both ends are everted and matured; proximal loop is usually everted to a greater height compared to the distal end
- End-loop ostomy: bowel is completely divided and proximal limb i sbrought through abdominal wall as loop with short efferent limb
- Jejunostomy
- Uses jejunum
- Stoma output: watery, bilious, high volume
- Indications: Crohn disease, trauma, ischemia bowel, or prior bowel resections
- Ileostomy
- Uses distal portion of small bowel
- Higher, more liquid output compared to colostomy
- Indications: inflammatory bowel disease, familial adenomatous polyposis, cancer, distal colorectal anastomosis
- Colostomy
- Uses any portion of the colon (usually in sigmoid or transverse)
- Less, more foul-smelling output compared to ileostomy
- Indications: cancer, Crohn disease, volvulus, fecal incontinence, trauma, congenital malformation, neurologic disorder)
- Urostomy
- Uses portion of ileum or colon as conduit, taking portion of bowel out of continuity and re-establishes intestinal continuity and using discontinuous loop as a conduit
Ostomy Site
- Considerations
- Posture
- Mobility
- Contractures
- Wheelchair use
- Walker use
- Examine the patient
- Evaluate the abdomen in supine, sitting, standing, and bending forward position in order to take note of creases, scars, skin folds, and valleys
- Note where patient wears belt
- Note rectus abdominis (ideal site is through this muscle)
- Location requirements
- Flat
- Visible to patient
- 2-3 inches lateral to midline incision
- Below the belt line (if possible, to allow for concealing the stoma → obese patients may require higher stoma as abdominal wall is thinner more superiorly)
- Ideally created within rectus abdominis muscle for increased support and stability
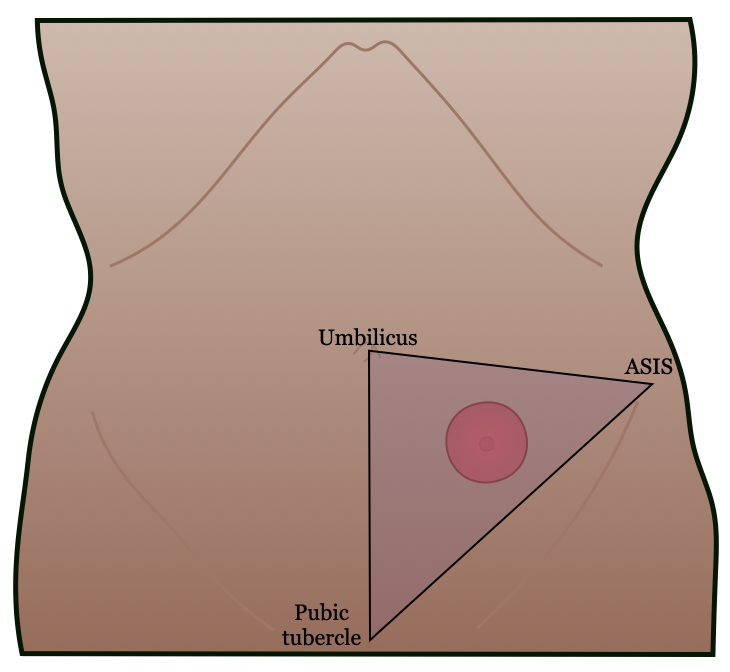
- Ostomy triangle → ideal location for ostomy placement
- Umbilicus
- Pubic tubercle
- ASIS
- Note: obese patients may be better suited to have ostomy located in the upper abdomen secondary to body habitus
Goals with Creation
- Small bowel stomas
- Protrude ≥2 cm above skin
- Will initially have high output with >1 L a day, but this should decrease as the bowel accommodates to increase fluid resorption and patients should expect 500-1000 cc output per day
- Thin output, little odor
- Colostomy
- Protrude 1 cm above skin
- Output amount varies depending on location
Ostomy Appliances
- Most appliances last 3-7 days; some are one-piece and some are two-piece
- Skin barriers
- Consist of pectin-like material surrounded by strip of adhesive
- Two-piece appliances will have additional plastic ring to which the puch can be attached
- Extended-wear models are designed to withstand more water output and may work better for ileostomy or urostomy, as these stomas have more liquid/watery output as well
- Skin barrier should match the contour of the stoma → they come either pre-cut or cut-to-fit
- Pouch
- Holds the effluent
- Available in either transparent or opaque material
- Either vented (i.e., contain charcoal filter to reduce odor) or nonvented
- Should be emptied when ⅓ to ½ full of liquid or gas
Peristomal Skin Care
- Most common cause of skin irritation is stool contacting the skin
Diet Modifications
- Diet modifications are not long-term
- Patients should chew food well and cut food into small pieces, abiding by a low-residue diet for 2-6 weeks postoperatively
- These modifications are recommended in order to avoid a blockage that presents with highly fibrous foods and can result in colicky pain with decreased ostomy output → treatment involves IVF, NPO, NGT, and irrigation of stoma
- Ways to avoid excess gas
- No smoking
- Do not use straws
- Eat slowly
- Do not chew gum
- Do not suck on ice
- Do not drink carbonated beverages
- Do not skip meals
- Do not eat gas-forming foods
- High ostomy output
- Defined as output >1L in 24 hours
- Treatment
- Increase PO fluid intake
- Each foods that thicken stool
- Applesauce
- Banana
- Tapioca
- Psillium
- Antidiarrheal medications
- Loperamide
- Diphenoxylate
Medications
- Prescriptions may need to be adjusted due to absorption changes
- Laxatives should never be prescribed for patient with an ileostomy
- Diuretics may need to be adjusted in patients with new stomas due to concern for dehydration
Lifestyle
- Activities patients can do with stoma
- Bathe
- Shower
- Swim
- Pregnancy
