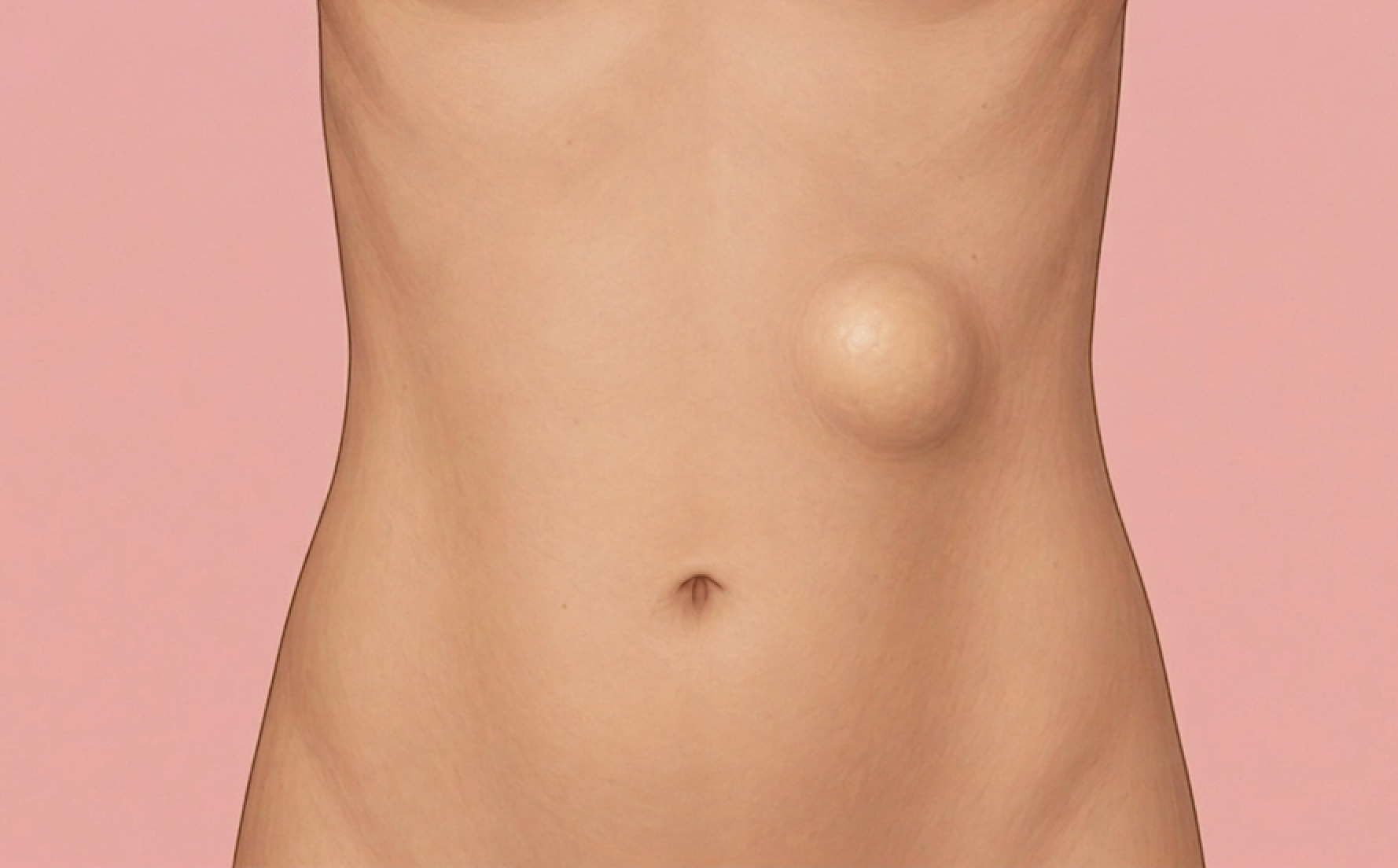
Tumors of the abdominal wall exist in abundance and are a common consult that general surgery receives.
Lipomas
- Typical lipoma
- Most common lipoma
- Benign tumor of adipose tissue with thin fibrous capsule
- Presentation
- Localized, encapsulated mass
- Occurs throughout the body, varies in size
- Majority occur in subcutaneous tissue, but can occur between muscle layers and within tendinous sheaths
- Usually painless, but can have mass effect with compressing symptoms
- Diagnosis is clinical
- Treatment
- Asymptomatic → observation
- Symptomatic, concern for malignancy, patient preference/cosmesis → excision
- Spindle cell lipoma
- Elongated spindle-shaped cells
- CD34+
- Fibromyolipoma
- Stellate dendritic processes in myxoid stroma with fibrotic spindle-shaped bundles and adipocytes
- Hibernoma (pseudolipoma)
- Abnormal growth of residual brown fat
- Brown fat is more common in infants → thighs, upper back, neck, arms
- Associated with 11q13 rearrangement → MEN1, AIP
- Chondrolipoma
- Mature adipocytes, adipoblasts, and mucus-transparent cartilage-like matrices
- Predilection for adipose tissue and skeletal muscle
- Angiolipoma
- Vascular tissue and mature adipocytes
- Can present with pain from the tumor which is usually due to thrombosis of the vascular structure → infarction and necrosis
- Extremedullary myelipoma
- Trilinear myelogenous cell development characteristic of bone marrow
- Familial multiple lipomatosis
- Rare autosomal dominant
- Multiple lipomas starting around age 30 and peaking at age 50
Neurofibroma
- Can be associated with neurofibromatosis
- Pathophysiology: benign nerve sheath tumors
- Presentation
- Diameter <2 cm
- Numerous lesions → sporadic, solitary lesions
- Raised, soft, skin-colored nodule <2 cm in size
- Button-hole sign → lesion retracts into skin when direct pressure is applied
- Diagnosis is clinical but may require biopsy
- Treatment
- Asymptomatic → observation
- Symptomatic or concern for malignancy → excision
Schwannoma
- AKA neurilemmoma
- Pathophysiology: pathologic growths of Schwann cells in neurologic sheath
- Presentation
- Usually occur in head and neck
- Circumscribed swelling
- Can create pain and discomfort if associated with swelling
- Histology
- Streaks of spindle-shaped cells and myxoid material
- S100+
- Treatment: resection is curative
Myxoma
- Rare myxoid tumor of skin and subcutaneous tissue
- Presentation
- May arise in individuals with Carney syndrome
- Usually arise sporadically
- Pedunculated skin-colored lesion
- Workup: no need for imaging or biopsy
- Treatment
- Asymptotic → observation
- Symptomatic → surgical resection
Dermatofibroma
- Pathophysiology
- Benign fibrous histiocytomas or common fibrous histiocytoma
- Arise from dermis
- Presentation
- Adults
- Firm solitary lesion
- Nontender, hyperpigmented, subcutaneous nodule
- Usually <1 cm and asymptomatic
- Diagnosis is clinical and may require biopsy if uncertain
- Treatment
- Asymptomatic → observation
- Symptomatic, concern for malignancy, patient preference/cosmesis → excision
Eccrine Spiradenoma
- Pathophysiology: arise from processes that differentiate the ductal and secretory cells of eccrine sweat glands
- Presentation
- Size 3 mm – 5 cm
- Painful
- Raised lesion blue, pink, or purple in color
- Histology
- Components of sweat glands
- S100+
- Treatment: surgical resection (due to concern for malignancy)
Desmoid Tumors
- Primarily composed of myofibroblasts, benign without metastasis
- Locally aggressive with high local recurrence
- Pathophysiology
- Arise from myofibroblasts
- Arise spontaneously
- Presentation
- Can be locally aggressive
- Associated with high recurrence rate
- Anterior abdominal wall
- Most common location
- Often occur during or after pregnancy, trauma, or surgery
- Deep seated, painless nonmobile mass often in fascial plane
- Intra-abdominal desmoid
- Associated with Gardner’s syndrome and retroperitoneal fibrosis
- Often encases bowel (difficult to perform resection)
- Diagnosis
- CT: depends on composition
- Can be homogenous or heterogenous
- Can be hypointense or hyperintense
- Core needle biopsy: spindle cells, dense fibrosis, high cellularity, low mitotic index
- CT: depends on composition
- Treatment
- Asymptomatic or stable size → observation can be observed
- Symptomatic → surgical resection
- Unresectable
- Neoadjuvant radiation can be considered in complex cases
- Chemotherapy (e.g., sulindac, tamoxifen)
- Imaging may be needed to evaluate relationship to abdominal wall
- Consider colonoscopy to evaluate for familial adenosis polyposis
Abscesses
- Collection of purulent fluid in dermis and subcutaneous tissue
- Etiology: bacteria → Staphylococcus (most common), Streptococcus, majority are polymicrobial
- Presentation
- Painful, fluctuant on exam
- Erythematous nodule
- May have surrounding cellulitis with associated induration
- Diagnosis
- Physical exam
- Ultrasound or CT if uncertain of diagnosis
- Treatment:
- Primary → surgical I&D
- Indications for antibiotics
- Size ≥2 cm
- Multiple lesions
- Extensive surrounding cellulitis
- Sepsis/systemic toxicity (fever, tachycardia, hypotension)
- Immunosuppressed (diabetes(
- Prosthetic devices
- High risk for endocarditis
- Failure of I&D
Cysticercosis
- Pork tapeworm
- Etiology
- Taenia solium (most common)
- Ingestion of larvae shed by parent worm into feces
- Presentation
- Cyst formation throughout the body
- Cysts in subcutaneous tissue
- Diagnosis
- Imaging
- Serology
- Cyst aspiration
- Cytology
- Treatment: medical management
Hydatid Cyst
- Echinococcal cyst
- Etiology
- Echinococcus granulosus
- Usually cycles between canines and farm animals
- Presentation
- Involves liver and lungs
- Slowly expanding mass with chronic discomfort
- Treatment
- Albendazole
- Mass observation for resolution
Epidermoid Cyst
- Sebaceous cyst
- Pathophysiology
- Benign subepidermal nodules
- Filled with keratin due to plugging of follicular orifice
- Presentation
- Most common cutaneous cyst
- Sporadic
- Found anywhere on body
- Ranges in size from 0.5 cm – 2 cm
- Central punctum present
- Usually asymptomatic
- Treatment
- Acute infection → incision and drainage
- After resolution of infection → curative excision